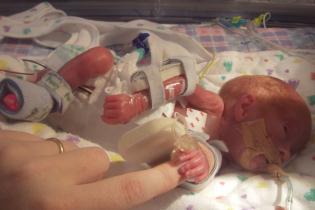

Linda
Mosaic Trisomy 16
Ours was a planned pregnancy with no initial worries. We did the 12-week Downs screening more to get a sneak peek at our foetus than because of any concerns or risk factors. So after the ultrasound was clear, it was a surprise two weeks later to hear that our blood tests had come back with a 1 in 50 chance of Downs Syndrome.
We considered our options, and were inclined to continue the pregnancy – but a CVS would likely put our minds at ease and confirm all was ok, so we did it. Two weeks later the obstetrician rang with the news of trisomy 16 in 10 of 11 cells – but it didn’t make sense. “This should be incompatible with life,” he said “but you’re still pregnant at 16 weeks so maybe the test was wrong.” We had an amnio, waited again, and began internet surfing to try to understand the potential consequences – there have been very few cases here in Australia. At this point the stories from DOC16 and several journal references were invaluable to us – and to our medicos – as a source of information.
At 18 weeks the results were back, clear of trisomy 16. Our ob had also done more research and advised that apart from a likelihood of early delivery because of our bodgy mosaic trisomy 16 placenta, our daughter’s life was likely to be pretty normal. The 20-week scan would be the final diagnosis tool, and would be supported by a meeting with a geneticist from the big city.
At 20 weeks (by our calendar dates, 19 weeks by the 12-week ultrasound dating), our foetus was the size of a 17 ½ week old and showed just a few ‘soft’ signs of genetic issues: an echogenic bowel, thickening of an area of muscle wall in the heart and a thickened placenta. The geneticist was optimistic for few medical problems, though the delay in growth indicated that an early delivery was likely. We would be monitored with 4-weekly ultrasounds, and do a tour of the NICU at our nearest city’s major hospital.
The following weeks brought joy as we felt baby move for the first time. Our 24-week scan showed us still 2-3 weeks behind in growth – at least we hadn’t fallen further behind. We prepared by completing our birthing classes and ordering a cot and car capsule.
As I passed week 25, we finally dared to believe that our baby would survive, albeit with a period of hospital care. But this was soon followed by a nagging pain in my ribs – yay I thought, my uterus is growing and my ribs are expanding. Paracetamol helped a bit, an osteopath visit relieved the pain entirely for a day, and I struggled on with less and less sleep thinking I’d tell the doctor at my 28-week scan.
Halfway through week 27 I gave up my determination and rang the hospital. I went in for a checkup, all the tests were coming back fine and we were even given dinner while we waited for the blood test results before going home. Then a doctor and nurses came in and our world turned upside-down.
I had HELLP syndrome, a severe form of pre-eclampsia that threatened not just baby but my life too. I hadn’t realised this was more likely because of our mt16, I guess my research had focussed on outcomes for the foetus rather than myself. My immune system had gone into self-destruct mode, my platelets were at 80 and I was at risk of uncontrolled bleeding. They administered a drip of magnesium to reduce my risk of seizure, and a steroid shot to help mature baby’s lungs. We waited through the night, listening to the heartbeat on the foetal monitor and looking at each other each time it slowed and then sped back up. I got a second dose of steroids at 12 hours, and the morning blood tests showed they had helped my platelets improve to a borderline 100. A caesarean under general anaesthetic would be performed.
I woke from the c/s to find a neonatologist sitting next to me with photos of my newborn daughter, and was clutching these as I was wheeled out to my husband. Linda weighed 555g (1 lb 2 oz), was 29cm long and had breathed on her own when ‘extracted’. I was fine.
I don’t remember much of the first couple of days, my husband’s comment was that she looked like a ‘skun rabbit’. His wedding ring fitted over her arm at the shoulder. I began expressing colostrum, and found that milk supply was one thing I could do very successfully – even if she could only have 0.5 mL at a time. Linda progressed: a hole between her arteries closed with the assistance of some drugs, she recovered from a bout of necrotising enterocolitis, and the typical retinopathy of prematurity issues never actually required surgery. She was very small and grew slowly, and was taken off breast milk at about 3 months old as she wasn’t digesting the fats thoroughly – her early intravenous feeds had blocked her bile ducts, and they needed time to clear out and return her digestion to normal. A low-fat formula improved her stools and her sleeping as her gut pain eased. She took some time to wean completely off oxygen and learn to bottle-feed, but was great at pulling her tubes and monitors off!
After 4 months and 10 days, we brought Linda home, weighing 2.2 kg. Having expressed to maintain some milk supply, I was able to wean her back onto full breastfeeding three months later. Soon she was rolling, then crawling, finally steps, words, climbing, jumping and great social relationships... nearly enough to forget how this all started!
Linda has remained small, but this hasn’t stunted her capacities. She’s a little behind in motor skills and speech, but not enough to require any specific catch-up therapy. I frequently get comments about how well she’s doing for her age, with people assuming her age relates to her size. She attends a wonderful local day-care, where we have gradually increased her hours as she’s improved her independence – at 2½ she does 4 mornings and one full day each week.
At birth, we felt we’d landed one of the poorest outcomes we could have hoped for. But nearly 3 years later we have one of the best, most ‘normal’ children we know. And the early challenges become forgotten as we deal with painting skills involving food and door handles that are now within reach. Yay!!!
Update August 2014
 Time flies, children grow, and our little Linda is now 6. Still little - her growth chart lines track along below the 1% line and mean that she'll always be shorter than her peers. But this is the only lingering outcome of her MT16, which began to fade from our lives when her 3 year old assessments came back "normal" (or even better than normal) - the first time we'd heard that prognosis since early pregnancy. This girl is intelligent, strong, socially capable and a very welcome part of our family - which has expanded to include two more "normal" children (after one early miscarriage). Perspective is a wonderful thing for us.
Time flies, children grow, and our little Linda is now 6. Still little - her growth chart lines track along below the 1% line and mean that she'll always be shorter than her peers. But this is the only lingering outcome of her MT16, which began to fade from our lives when her 3 year old assessments came back "normal" (or even better than normal) - the first time we'd heard that prognosis since early pregnancy. This girl is intelligent, strong, socially capable and a very welcome part of our family - which has expanded to include two more "normal" children (after one early miscarriage). Perspective is a wonderful thing for us.
